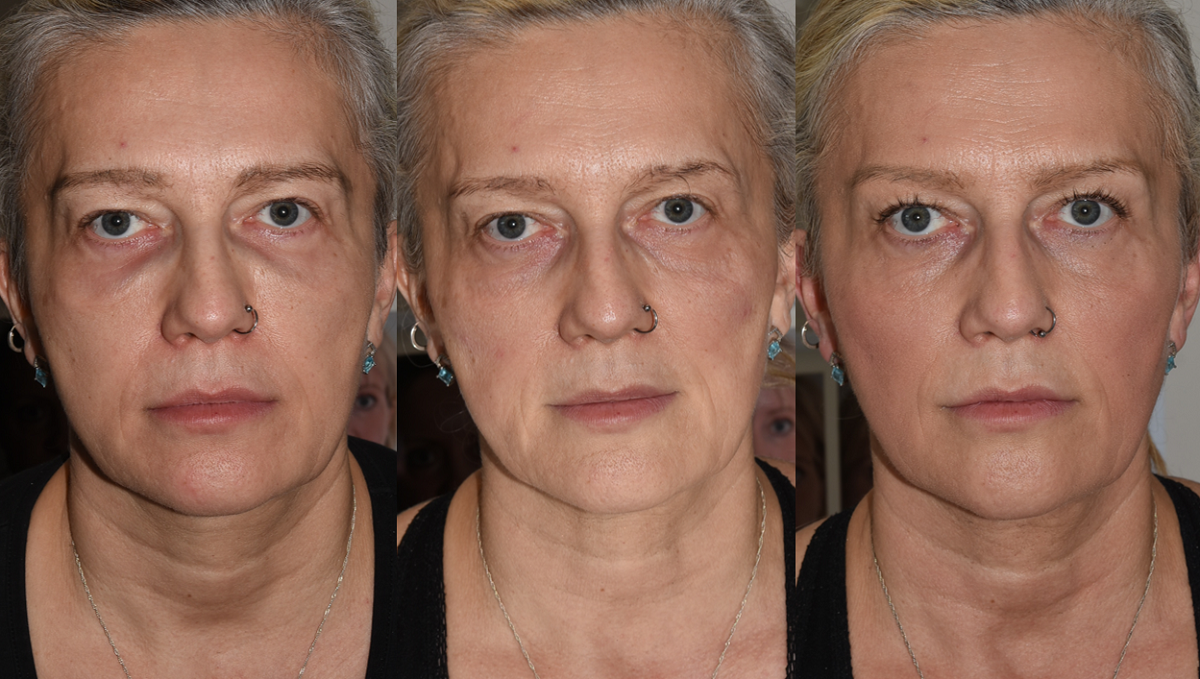
From Botched to Beautiful: The Journey of a Filler patient
10th August 2021
2021: 4 takeaways from my dermatology and cosmetic practice
26th December 2021A CQC inspection is when the Care Quality Commission (CQC) visits health and social care services, such as hospitals or care homes, to check the quality of care provided. The CQC ensures that services meet standards of safety, effectiveness, care, and leadership.
During the inspection, inspectors look at how well patients are treated, how staff are managed, and whether facilities are safe. Afterwards, they rate the service as Outstanding, Good, Requires Improvement, or Inadequate. These inspections help keep services accountable and ensure people receive the best care possible. Regular CQC inspections also encourage continuous improvements in care quality.
I have just had a comprehensive CQC inspection. Eventually, it went well and I have earned an overall GOOD rating, but it took a lot of stress during a very difficult COVID year to get prepared and get through.
When finished, I spent a couple of hours putting together a list of items needed for a successful inspection. This list would have been a great help for me, and I hope it will help other similar private doctors to get prepared for their inspections.
So, this list is here for you to consider. It reflects my personal understanding at the time of writing. I am sure it is not complete, so you need to do your own due diligence. If you find it useful and there are things you can add or amend, please let me know in a comment below, so we can keep it fresh and useful together as time passes.
How to get prepared for a comprehensive CQC inspection?
(this document reflects my best understanding after my recent comprehensive inspection in Nov 2021)
Required content may change if the practice provides NHS services, mobile services, online services, use controlled drugs or works at satellite locations, etc. I don’t.
Documents needed:
– book of policies with risk assessment documents (list of my policies and risk assessments are attached)
– accident book with a template on how to record an event
– statement of purpose document
– Practice mission/vision/values statement document
– Chaperon policy sign on the wall
– Complaints leaflet available for patients
– medicine fridge daily temperature check evidence (double thermometer applied)
– proof of ID checks of new patients (especially if they come with a minor or vulnerable person)
– notable practice document (how is the practice safe, effective, responsive, well-led and caring. Presentation of these points via live examples/actions from the practice.)
Important subject to cover and be prepared to show readiness and evidence:
– provide an overview of the changes made in response to COVID (or any other actual major event)
– Safety and drug alerts process and evidence of management and actions (MHRA alert subscription, follow up and action)
– Summary of significant events recorded in the past 12 months
– Summary of complaints recorded in the past 12 months
– Evidence of learning shared, and improvements made (meeting minutes of in house staff meeting and training)
– yearly patient satisfaction survey, results and actions taken
– emergency medicines are easily accessible and within expiry
– know your patient numbers, composition, referrals (consent for referrals)
– the clinic’s communication with patients’ GPs
– Where the service excels?
– Areas of challenge?
– Medicines management (prescribing and administration)
– Benchmarking: measurement of service against other services. For example, how does this organization compare with similar organizations that provide the same services?
– Clinical records of patients (storage, access, prevention of loss or breach, ID check, allergies, medications and consents are recorded, sharing with GP), ICO registration
Building related documents, risk assessments and actions (evidence)
It is the responsibility of the registered manager to recruit these documents and follow up on the recommended actions
– Fire safety/health and safety policies
– Latest fire risk assessment and any action log
– Evidence and date of fire extinguish check
– Evidence of the latest fire drill and any actions taken
– Latest health and safety risk assessment and any action log
– Latest legionella assessment
– Equipment calibration dates and copy of the certificate
– PAT testing dates and copy of the certificate
– Latest Infection prevention control audit and action log
– Defibrillator (everybody knows where it is, clearly labelled on the wall, pads within expiry!)
– emergency oxygen and proof of service, pulsoxymeter, thermometer, blood pressure monitor
Audits (two cycles: audit and re-audit)
– list of audits needed are detailed in the Quality management and good governance policy
– prescribing audit (by doctors)
– cleaning audit
– Infection prevention control audit (by IPC lead)
– treatment outcome audits (by doctors, whether the treatment outcomes of the clinic meets standards. Also see: benchmarking)
– any independent audits?
Training – role-specific: (frequency and level are individual according to the role)
– Adult/child safeguarding
– Fire safety training
– chaperon training (a member of staff with this training is always available if needed)
– Information Governance and Data Security training
– Mental Capacity
– Infection Prevention and Control
– Resuscitation/BLS/First Aid
– Health and Safety
– Manual Handling
– Equality and Diversity
– Whistleblowing
HR:
– related policies (see list of policies)
– Induction process
– Training policy
– Recruitment policy
– Record of DBS checks for staff (including reference number)
– proof of immunizations
– proof of yearly appraisals, governing body membership
– The number of sessions or hours worked by each staff member
– A selection of staff files including any recruited in the last six months reflecting evidence of staff appraisals, 121/supervisions, inductions, proof of identity, DBS checks, references, qualifications.
– Staff training records
For GPs only:
– Policy and process for the management of repeat prescriptions and medicine reviews
– Cold chain policy and audit
– Policy/process to ensure information is shared with others such as coding of medical records
– Online services policy
Useful links:
https://www.cqc.org.uk/guidance-providers/gps/gp-mythbusters-full-list-issue-number
https://www.bma.org.uk/media/1598/prepare-for-a-cqc-inspection-guidance-and-appendices.pdf