Dr Bela, Dermatologist, Mole Check in West London
Dr Bela’s experience with moles, skin cancer, and melanoma puts him among the top few. Throughout his mole clinic franchise, 8000 screenings are performed yearly an average. As the ultimate quality assurance, he approves all mole removal cases and answers consultation requests from his fellow doctors daily. This way the number of moles and melanomas he sees regularly is significant. You can have peace of mind when he checks your moles.
Everybody can have skin cancer, but the relative risk can be defined by the following factors. The more you tick the higher your risk:
- high number of moles
- high number of asymmetrical moles
- melanoma in the personal or family history
- being sunburnt in the past
- immune suppressive treatments
Also, the risk for skin cancer increases with age.
If you are interested in online mole check please CLICK HERE.
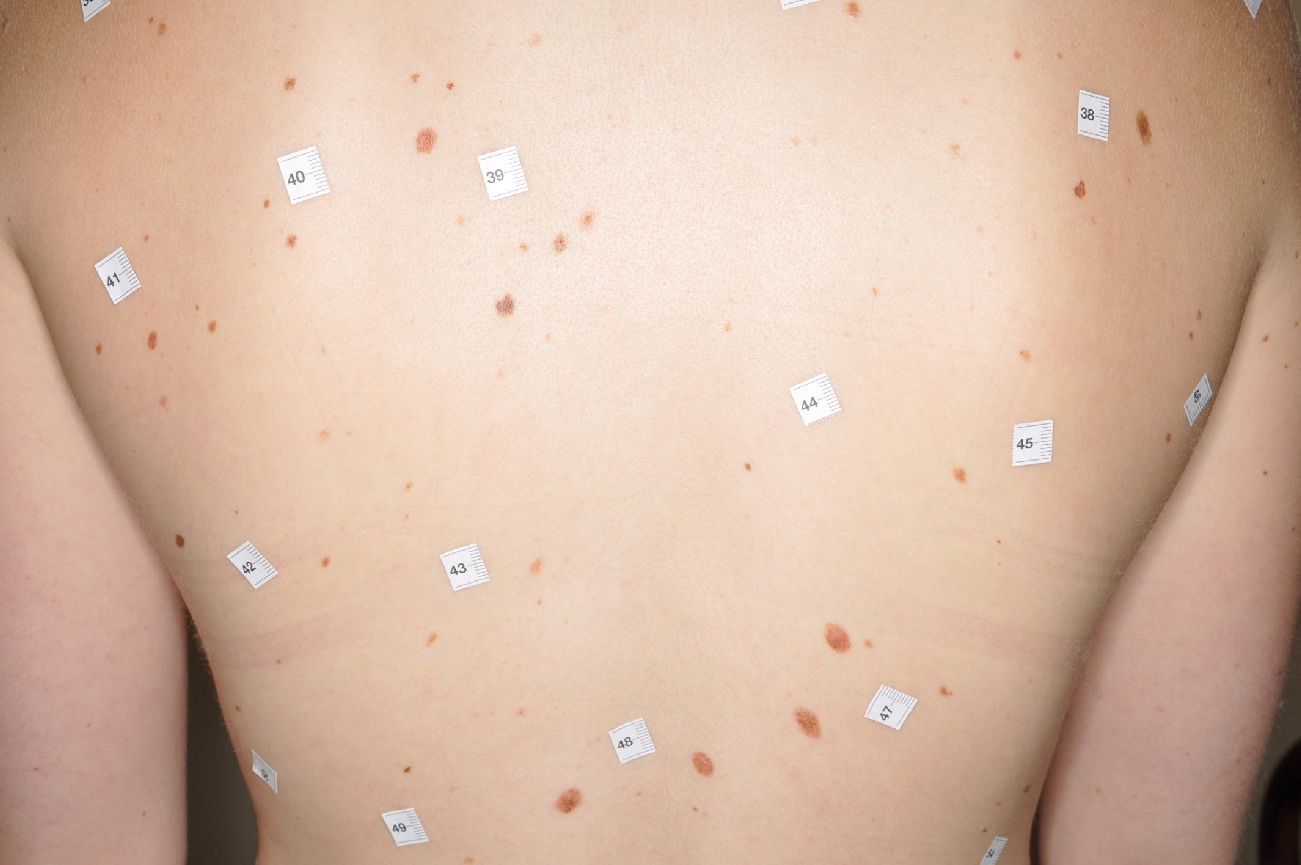
If you have a mole which is new or changing in size, colour or shape that might be suspect for melanoma skin cancer and should be checked immediately. Also, bleeding of a mole without injury can be a sign. Book an appointment straightaway!
If you are interested in online mole check please CLICK HERE.
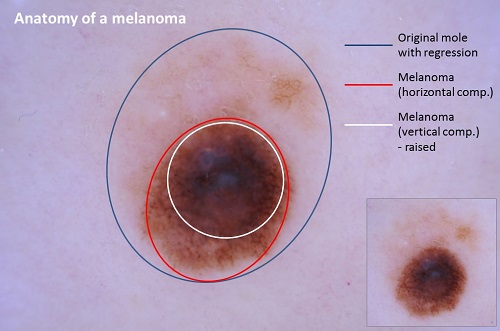
Put it simply: it can save your life. Based on the analysis of our 63.000+ screenings 43.7% of melanoma patients of our mole clinic could raise the growing tumour as a complaint during their mole check. The majority of the patients though (56.3%!), did not notice anything suspicious. Mole check is about detecting an early stage skin cancer when the removal results in 100% cure.
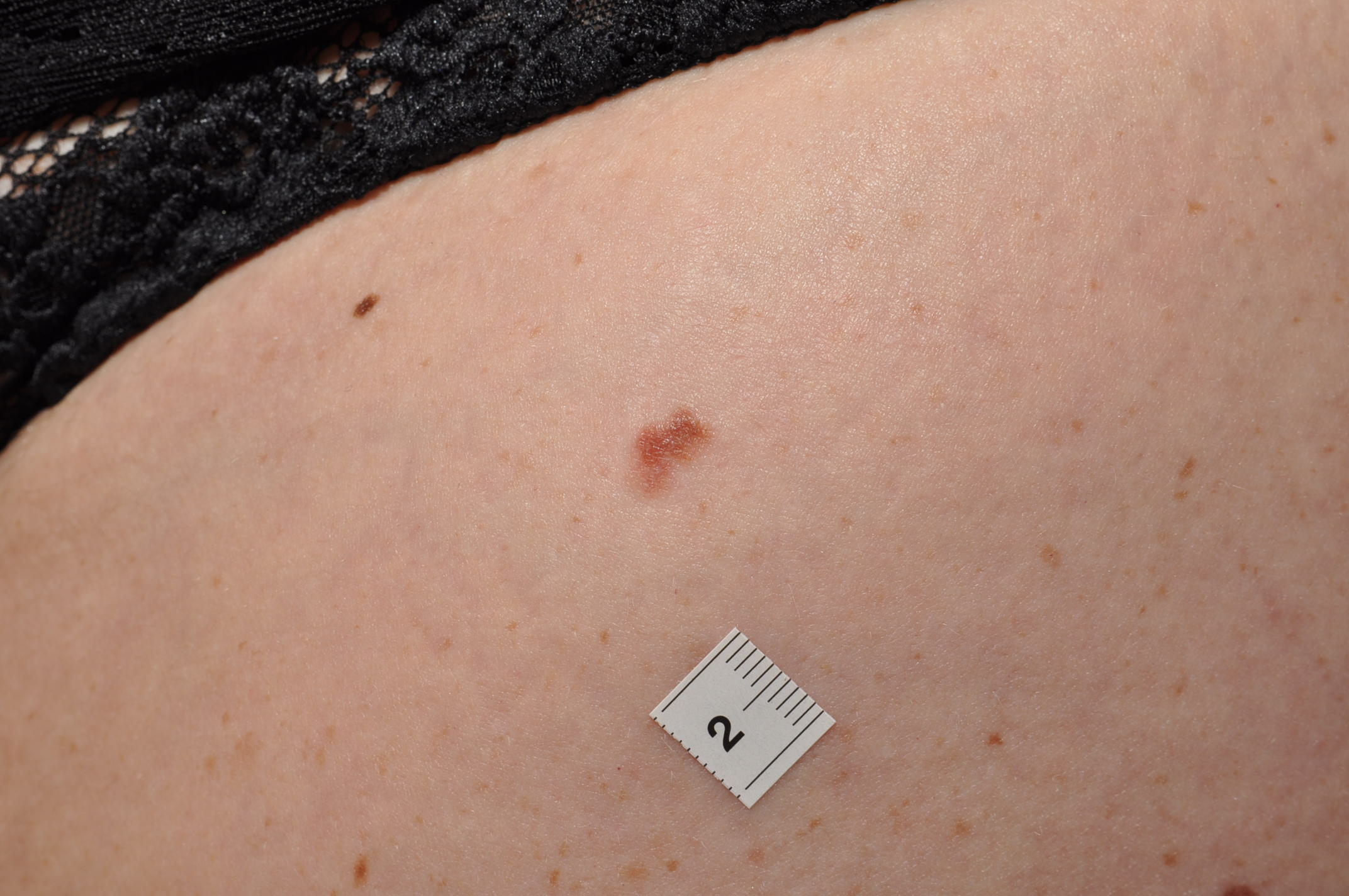
Initially, melanoma growth in the top layer of the skin (epidermis) where it originally develops from pigment-producing cells (melanocytes). Since there are no blood vessels in this layer melanoma cannot spread. If it is cut out at this stage the cure is 100%.
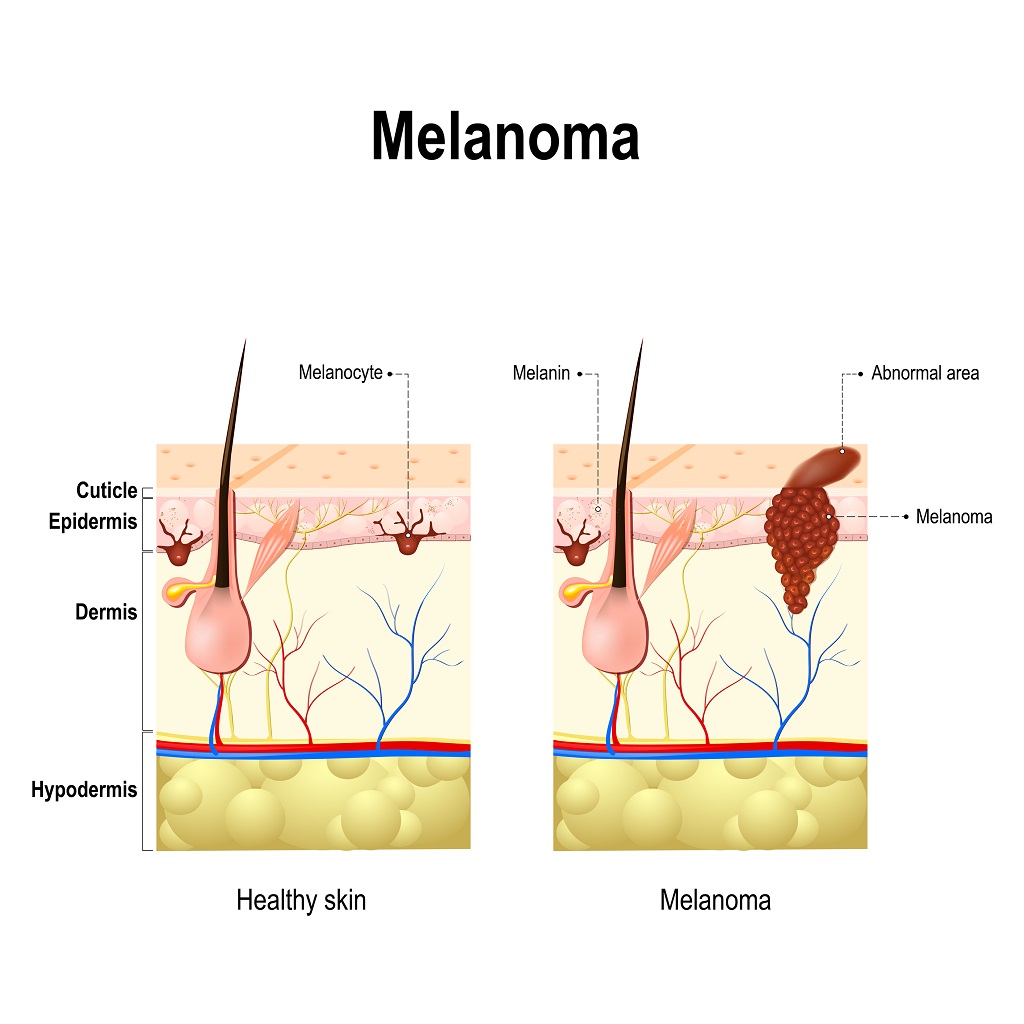 After a certain time (usually years) the melanoma starts to grow vertically. Once it reaches the dermis (the layer of the skin where there are blood vessels) it can spread to distant parts of the body and can become incurable. So, at the time of the removal of the visible tumour, there might be invisible cells migrating away from it via lymph and blood vessels. The thicker the tumour is, the higher the chance of this happening, so these cells are left behind during surgery. Typically, in 2-5 years time then, these cells form new tumours (metastases) at distant locations and potentially can prove lethal.
After a certain time (usually years) the melanoma starts to grow vertically. Once it reaches the dermis (the layer of the skin where there are blood vessels) it can spread to distant parts of the body and can become incurable. So, at the time of the removal of the visible tumour, there might be invisible cells migrating away from it via lymph and blood vessels. The thicker the tumour is, the higher the chance of this happening, so these cells are left behind during surgery. Typically, in 2-5 years time then, these cells form new tumours (metastases) at distant locations and potentially can prove lethal.
Melanoma malignum is the deadly type of skin cancer. It can originate from pre-existent moles or it can appear as a new lesion on the intact skin. While in the early (horizontal growth) stage it looks like a normal mole that is why it is very difficult to detect. When it starts to grow vertically into the deep layers of the skin, it becomes dangerous and it can spread through the vessels to distant locations (metastasise) becoming incurable.
Melanoma should be found and removed as early as possible. Screening can save your life.
Skin cancer is a group of cancers originating from the skin. The deadly melanoma and the more benign baso- or spinocellular carcinomas belong here. You don’t need to know this classification; when you come for a mole check or skin cancer screening, we are looking for all of them.
Melanoma grows slowly and the detection of this change can be challenging even for professionals. The comparison of moles at different times can improve the diagnostic accuracy because the size and different structural features can be compared to baseline pictures and the changes can be assessed more objectively.
Mole mapping means the one-by-one recording of all moles, the comparative analysis of pictures to previous stages and most importantly it gives the opportunity of multiple independent assessments, as it happens at MelanomaMobil, where 2-3 different doctors check the moles of a single patient routinely.
The image below shows a case when the melanoma was missed by both the patient and the screening doctor and was detected by the evaluation doctor (who gives a second opinion based on the pictures). You can see the change on the close-up and high magnification pictures compared to the ones taken a year before.
Mole mapping is the gold standard in melanoma screening.
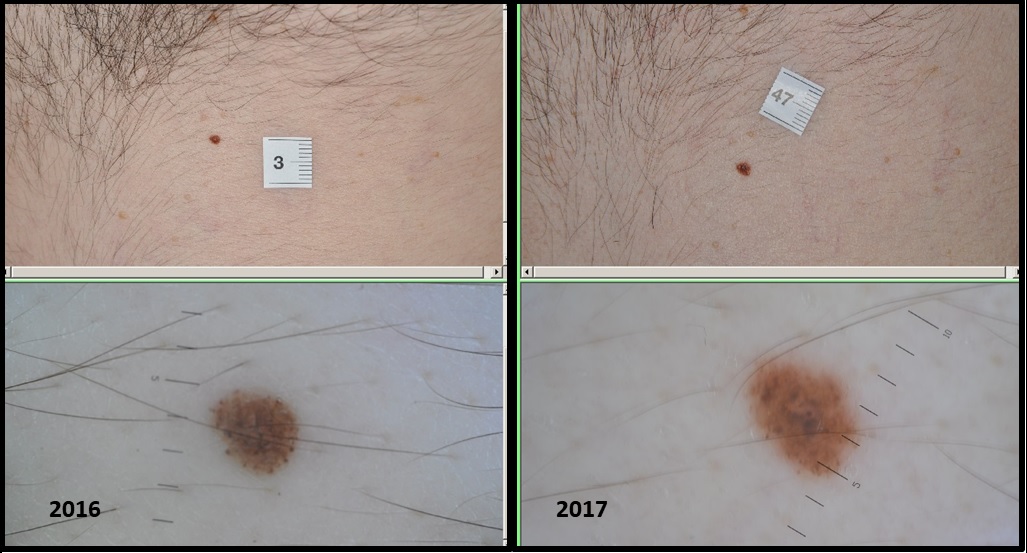
Comparative analysis of moles is when moles are assessed and compared to baseline recordings (mole map) taken at earlier times. This way potential changes in size, shape, pigmentation and sub-structures can be assessed more objectively which improves diagnostic accuracy.
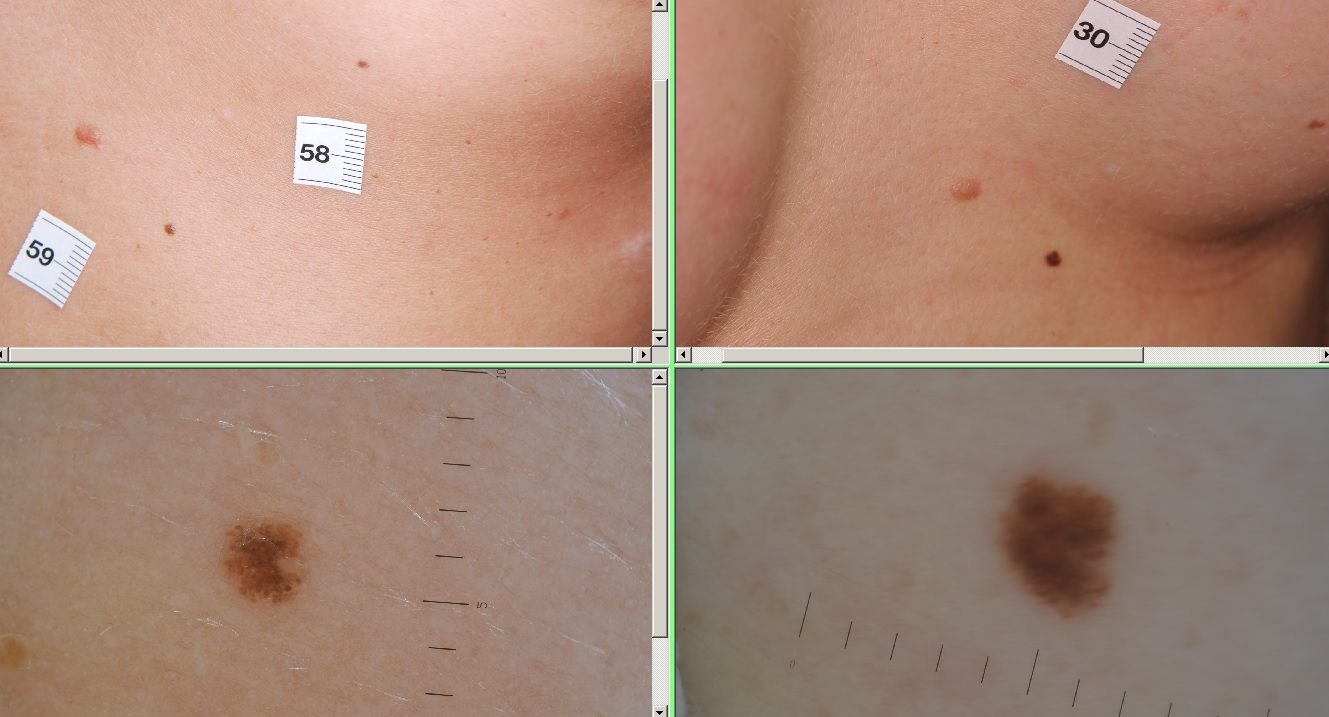
Mole mapping and comparative analysis of moles is the gold standard of melanoma screening. Analysis of our own data based on 63.000+ screenings shows that 36.2% of all melanomas were diagnosed by comparative analysis so that these melanomas were missed by the patient and the screening doctor.
This is the most important take-home message for lay people. Ugly duckling sign is when one of the moles is different from the rest: it is darker, more asymmetrical, bigger or growing. If you have a mole which differs from the others, or you see one on someone’s skin, it should be checked out immediately at our clinic.
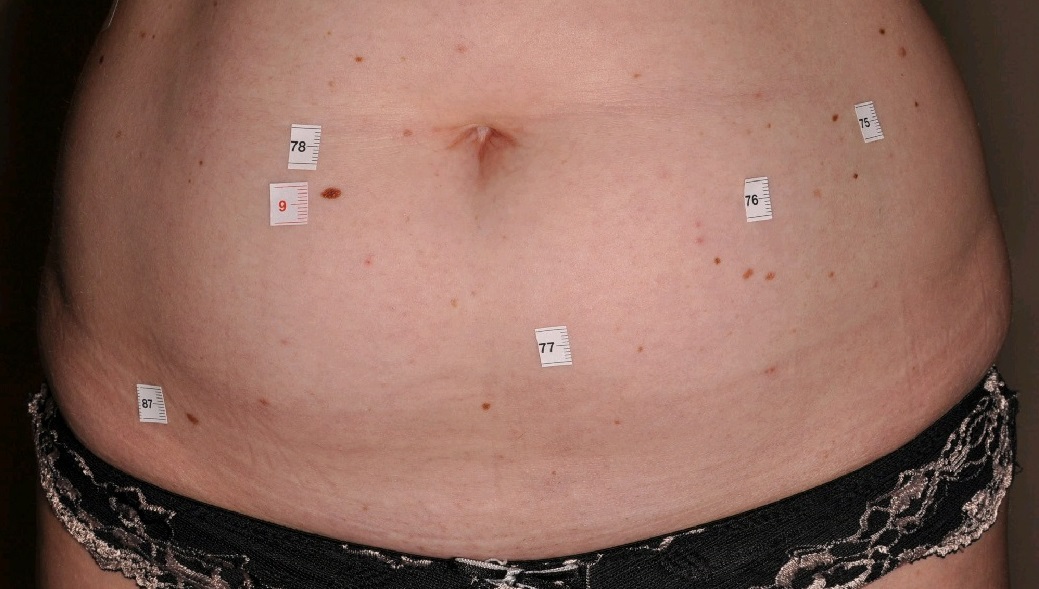
Based on our own research, 43.7% of our melanoma patients complained about the lesion which turned out to be melanoma. It means that less than half of the patients of our mole clinic had a suspicion at all and in the majority of cases they didn’t have a clue; the melanoma was found by a professional.
So, how to spot a melanoma? It can look different from the rest of the moles (ugly duckling sign), can be darker or bigger. It can be the most asymmetrically shaped or the darkest one and it can grow slowly. If you have any suspicion it should be checked by a professional.
Would you recognise this early stage melanoma?
If you are interested in online mole check please CLICK HERE.
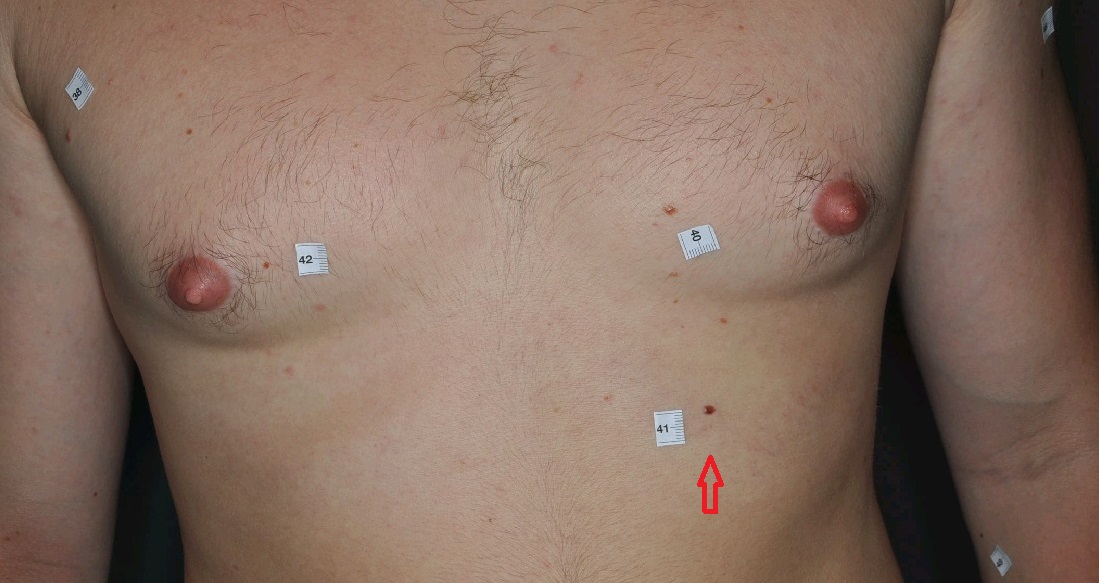
Melanoma is curable while in its early stage. Initially, melanoma growth in the top layer of the skin (epidermis) where it originally develops from pigment-producing cells (melanocytes). Since there are no blood vessels in this layer melanoma cannot spread. If it is cut out at this stage the cure is 100%.
After a certain time (usually years) the melanoma starts to grow vertically. Once it reaches the dermis (the layer of the skin where there are blood vessels) it can spread to distant parts of the body and can become incurable. The earlier the diagnosis and removal is, the better the chances for survival.
Everybody has a different level of inherited risk. Melanoma in the family history or high number of moles and atypical moles make the risk high to start with. Then sunbathing, use of artificial tanning beds and especially burning by any of these makes the risk even higher.
So, while one cannot do anything with the inherited risk, the extent of harmful UV radiation can be controlled by avoidance or use of proper sun protection.
For those with high risk, regular screenings are paramount.
The frequency of follow up mole checks depend on your individual risk. Dr Bela will recommend you a follow-up date based on your examination between 1-3 years.
A mole check without mole mapping is £180
A mole check with mole mapping (initial consultation) is £250.
Follow-up mole check with mole mapping: £250-315. The PRICE and TIME NEED for the examination depends on the number of your moles. It is stated in your individual follow-up reminder email.
Please book your time accordingly!
|
Your S category |
Time to book |
Price |
|
S1-S2 |
45 min |
£250 |
|
S3 |
45min |
£255 |
|
S4 |
45 min |
£275 |
|
S5 |
45 min |
£295 |
|
S6 |
1 hour |
£315 |
Posting a CD with the images taken (admin charge): £15

